For diseases of nerves and muscles.
Why am I being sent to the EMG Lab for tests?
You are being sent to the electromyography (EMG) lab because you have numbness, tingling, pain, weakness or muscle cramps. Some of the tests that the EMG doctor may use to diagnose your symptoms are nerve conduction studies (NCS) and needle EMG. The EMG doctor will examine you to decide which tests to do.

Electrodiagnostic medicine is the study of the diseases of nerves and muscles. If you have been referred to our clinic, your doctor has recommended an EMG test to see if your muscles and nerves are functioning normally. The results of the tests will help your doctor decide what is wrong and how it can be treated.
Doctors who do EMG testing have completed special training, and work as Physiatrists (CAPMR). The doctor who completes your test should be certified either by the CSCN (Canadian Society of Clinical Neurophysiologists) or the AANEM (American Association of Neuromuscular and Electrodiagnostic Medicine).
Most patients coming for nerve testing will have nerve conduction studies (NCS). Many patients will have a second part of the testing called electromyography (EMG).
We specialize in the diagnosis and management of:
- Carpal Tunnel Syndrome
- Ulnar Neuropathy (e.g. Cubital Tunnel Syndrome)
- Foot drop (Peroneal Neuropathy)
- Traumatic nerve injury
- Polyneuropathy
- Spinal nerve injury in the neck or back (Cervical and Lumbosacral Radiculopathy) (AKA “sciatica”)
- Brachial plexus injury
- Muscle Diseases (Myopathy or Muscular Dystrophy)
- Motor Neuron Disease
- Amyotrophic Lateral Sclerosis
- Kennedy’s disease
- Myasthenia Gravis
We offer comprehensive management in:
- Carpal Tunnel Steroid Injections
- Spasticity management after stroke, traumatic brain injury or spinal cord injury including Botox injections (chemo denervation)
- Ultrasound guided spinal injections (caudal epidural)
- Medical management of autoimmune nerve diseases and myasthenia gravis
- Rehabilitation management for neuromuscular conditions.
Best practices by:
Davyd Hooper, MD, FRCP, DIP. CSCN, DIP. ABEM
Dr. Hooper completed his specialty training in Physical Medicine and Rehabilitation at the University of Manitoba in 2007 and joined the Clinic in July 2008 upon completion of his fellowship in neuromuscular and electrodiagnostic medicine at McMaster University.
He concurrently specialized in diagnostic nerve ultrasound and muscle biopsies during his fellowship. He is dually certified in EMG by the Canadian Society of Clinical Neurophysiologists and the American Board of Electrodiagnostic Medicine. He is an assistant professor at the University of Manitoba and is the Undergraduate Program Director for Physical Medicine and Rehabilitation for the University of Manitoba Medical School. He is also the Program Lead for the Neuromusculoskeletal Rehabilitation Program at the Health Sciences Centre. His research interests include the use of Ultrasound for the diagnosis of nerve and muscle diseases, as well as carpal tunnel syndrome management.
Sepideh Pooyania, MD,FRCPC,CSCN

Dr. Pooyania completed her specialty training in Physical Medicine and Rehabilitation at the University of Manitoba in 2009. She is certified in Electrodiagnostic Medicine by the Canadian Society of Clinical Neurophysiologists. Dr. Pooyania is the Service Chief for Stroke Rehabilitation at Riverview Health Centre and is an associate professor at the University of Manitoba.
Jennifer Salter, MSc,MD,FRCPC,CSCN
Dr. Salter completed medical school and a Master of Science in Human Biodynamics at McMaster University. She completed her specialty training in Physical Medicine and Rehabilitation at the University of Manitoba in 2012. Dr. Salter is certified in Electrodiagnostic Medicine by the Canadian Society of Clinical Neurophysiologists. She is an assistant professor with the University of Manitoba, Residency Program Director for Physical Medicine and Rehabilitation for the University of Manitoba Medical School and Service Chief for the Acquired Brain Injury Program at Riverview Health Centre.
Justin March
Dr. March completed medical school and residency training in Physical Medicine and Rehabilitation at the University in Manitoba, becoming a fellow of the Royal College of Physicians and Surgeons of Canada in 2019. He is certified with the Canadian Society of Clinic Neurosciences in EMG and NCS. His research interests include virtual reality in the treatment of phantom limb pain and mental health outcomes after major trauma. He is currently the team physician for the Winnipeg Rifles football team.
Lindsey Woodrow

Dr. Woodrow completed medical school and residency training in Physical Medicine and Rehabilitation at McMaster University, becoming a fellow of the Royal College of Physicians and Surgeons of Canada in 2019. She completed fellowship training in Cancer Rehabilitation Medicine at MD Anderson Cancer Center in Houston, Texas and joined the University of Manitoba Section of Physical Medicine and Rehabilitation as Assistant Professor in 2020. Dr. Woodrow is certified in Electrodiagnostic Medicine by the Canadian Society of Clinical Neurophysiologists. Her research interests include exercise as medicine and prehabilitation in cancer patients and using prognostic tools to aid in cancer rehabilitation goal setting.
Directions to the EMG Clinic
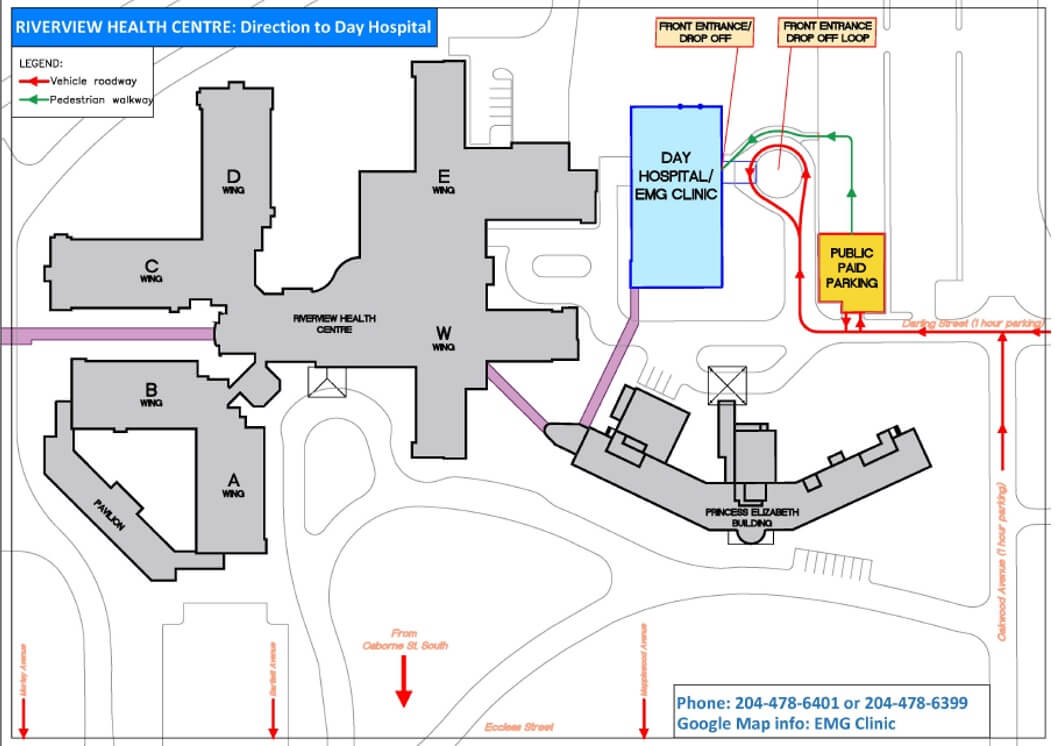
EMG Clinic is located inside the Day Hospital. Three maps have been included below, which include directions on how to get to the Day Hospital from our public parking lot and from parking on the street nearby. To locate Day Hospital using google maps: click on directions.
Your Questions
How long will my EMG tests take?
The tests usually take 40 to 90 minutes depending on the complexity of the testing. You can do any of your normal activities, like eating, driving, and exercising before the tests. There are no lasting side effects. You can also do your normal activities after the tests.
How should I prepare for my EMG tests?
Tell the EMG doctor if you are taking aspirin, blood thinners (like Coumadin), have a pacemaker, or have hemophilia. Take a bath or a shower to remove oil from your skin. Do not use body lotion on the day of the test. If you have myasthenia gravis, ask your EMG doctor if you should take any medications before the test. It is helpful if you bring clothes to change into so that you can be examined by the doctor (i.e. shirt if it is a hand problem, shorts if it is a leg problem).
How will I be informed of my EMG test results?
The EMG doctor will discuss your test results with you or send them to your regular doctor. After the exam, check with the doctor who sent you to the lab for the next step in your care.
What are some of the tests performed in the EMG clinic?
Nerve Conduction Studies: These tests show how well the body’s signals are traveling to a nerve. This is done by applying small electrical shocks to the nerve and recording how the nerve works. These shocks cause a quick, mild, tingling feeling. The doctor may test several nerves.
EMG(Electromyography): For this part of the test, a small, thin needle is inserted into several muscles to see if there are any problems. A new needle is used for each patient and it is thrown away after the test. There may be a small amount of pain when the needle is put in. The doctor tests only the muscles necessary to decide what is wrong. During the EMG test, the doctor will be able to hear and see how your muscles and nerves are working by analyzing the electrical signals in the muscle.
Where is the EMG Clinic located?
The EMG Clinic is located on the main floor of the Day Hospital at Riverview Health Centre. The Day hospital is located on the corner of Oakwood Avenue and Darling Street. There is a public paid parking located next to the Clinic.
There is also street parking nearby, but be aware of the parking signs as many streets are limited to 1-hour parking.
Click on the following map to enlarge and print.
Why am I being sent to the EMG lab for tests?
You are being sent to the electromyography (EMG) lab because you have numbness, tingling, pain, weakness or muscle cramping. Some of the tests that the EMG doctor may use to diagnose your symptoms are nerve conduction studies (NCSs), or needle EMG. The EMG doctor will examine you to decide which tests to do.
Key Contact
For more information contact us at:
Neuromuscular & Electrodiagnostic Clinic at 204-478-6399 or 204-478-6401
Clinic Nurse: 204-478-6155
Fax: 204-478-6409

